Last Tuesday, I gave a talk at the UCT medical school on the ethics of social media for medical professionals, which focused in part on the Health Professions Council hearings with regard to the ‘unprofessional conduct’ of Prof. Tim Noakes.
While I’ve presented a half-dozen or so talks on the philosophy and ethics of science for dietitians in the last couple of years – usually for continuing professional development (CPD) points – this one attracted more than the usual amount of attention, thanks to the imminent resumption of the Noakes hearings.
So much so, in fact, that I’ve been told that Noakes himself requested that I be instructed to not talk about Noakes or the hearings. Which is odd, seeing as I planned to – and did – speak in favour of Noakes with regard to his case that’s currently being heard in Cape Town.
With two days of the hearings now (nearly) complete, it seems a good time to summarise the gist of my talk, focusing especially on the Noakes hearings bit, seeing as that’s what’s being discussed in the media. But this is to some extent a restatement of a position I’ve put previously, which is that I don’t find his tweet actionable by the HPCSA.
As usual, I didn’t stick to my notes while talking, so if you happen to find a recording of the talk somewhere, don’t expect the text and the recording to map neatly onto each other.
Social Media Ethics for Medical Professionals
Our conduct on social media should largely be a matter of common sense – but common sense, as you no doubt know, is anything but common.
One could adopt a simply principle such as: “act just like you would in ‘real life'” (assuming you’re not deranged). This covers most of our lapses in judgement on social media, such as butting into conversations without invitation, or giving unsolicited advice.
But because common sense is uncommon, we make rules to govern behaviour. And this is the problem with professional ethics: it can lead to rule-following, rather than a promotion of key virtues.
Something can be unethical even though it doesn’t break any rules – for example, it might be unethical to offer certain forms of medical advice on Twitter, and the rules covering that might not yet have been written.
This is why we require the ability to engage in ethical reasoning – did I make the best possible choice, under the circumstances, even if no choice was perfect? (And for doctors or dietitians on social media, there is often a zero-risk option available, which would be to simply stay off social media!)
Before taking a look some general principles regarding the ethics of social media, let’s recap some history, as a reminder of how physicians are guided with regard to ethics in general.
In the 4th century BCE, Hippocrates, a physician-philosopher, directed physicians “to help and do no harm” (Epidemics, 1780). Alongside that, general ideas regarding respect for persons, autonomy (free choice) and for justice have been fairly constant concerns in the evolution of our societies.
Jumping ahead to modern times, a key development came in 1979, when the Belmont Report was released, dealing with how we should protect the interests of human subjects of research.
The report was written in the wake of the Tuskegee study (1932 – 1972), which involved over 400 poor African-American men who were denied treatment, without informed consent, for their syphilis.
The Belmont Report was written in large part by a philosopher, Tom Beauchamp, and it outlined 3 principles – respect for persons (i.e. autonomy), beneficence and justice.
Also in 1979, Beauchamp and James Childress published a text book – Principles of Biomedical Ethics – in which they adopted the three principles listed above and also added a fourth principle, that of non-maleficence.
I read this book as an Honours student in philosophy back in 1993, and it’s still being widely read and prescribed today in its seventh edition.
Of the four principles, the two that seem most relevant – along with some broad and important consequences of those principles for medical professionals on social media – will now be discussed.
Respect for Autonomy
Any robust notion of moral decision-making assumes informed and voluntary decisions (within reason, of course – we can’t ever have perfect information, and for some of us, including me, “voluntary” decisions are largely a fiction).
For decisions about our health, then, we’re assuming that decisions are made intentionally, in understanding of the options available and the relative risks accompanying those options, and without undue external influences that could be said to undermine a free choice.
The “informed” is key here – you, as a medical professional – know that you’re in a position of relative authority, and that you are granted a certain respect or trust, even in an age where “Doctor Google” consults to everybody.
What this means, by extension, is that you need to be wary of contributing to the echo chamber. You need to try to remain objective, and remember to alert people to issues of controversy, differing points of view, contested areas in your own fields, even if you have strong convictions. Especially if you have strong convictions.
A confounding element here is the tension between paternalism and authoritarianism. You might think it overly paternalistic to need to warn someone about every possible controversy, and I think you’d be right if you thought that.
There’s a responsibility on the part of the audience to do some research also, including not only the issue in question, but also who they are getting the advice from. It doesn’t take much work to figure out that Dr. Mercola is a quack, for example, and it’s to some extent your fault if you take him seriously.
The Principle of Nonmaleficence
This principle requires that you don’t intentionally create harm or injury, either through acts of commission or omission. Basically, this is about exposing people to unreasonably risk of harm.
The connection to social media here is that any good scientist would not speak in the language of absolutes, and that, if you’re recommending something where there is the possibility of risk, you’d include that in your tweets (not doing so would be a harm of omission).
This is my central thesis, which also asks you to remember the earlier point about rules versus ethical reflection: there’s a harm in encouraging dogmatic and sloppy thinking about science, because it increases the chances that people will make poor decisions about their health.
If you want to be an ethical practitioner, you shouldn’t mistake your conviction that you are right with the fact of you being right – because you’d know (right?) that this isn’t how science works. You’d know that science progresses by increments, with our discovering error, and that certainty isn’t something we can claim.
Saying that you are certain – or not alerting patients to views that are critical of yours – misrepresents the scientific method, and does harm to our ability to reason our way through scientific issues, and potentially (when we reach the wrong conclusions) our health.
My concern, then, is with subtle damage, and in particular damage to good scientific practice and epistemic virtue. Healthcare professionals have a particular duty in this regard, and it’s also an ethical concern, seeing as public misunderstanding of science leads, for example, to travesties like anti-vaccination or anti-GMO scaremongering.
The HPCSA professional guidelines make the requirement for ethical reasoning explicit, and call for it to be grounded in an overall concern for virtues like tolerance, truthfulness and compassion.
The problem for those of us on social media is the context, which encourages echo chambers and groupthink. So it’s important to think not only think about the conversation you’re having, but also who the listeners or observers are. Joe Bloggs might know what you mean, but people on the sidelines might walk away with a very confused idea of what they should eat, or what medicines they should be taking.
Some (boring) specifics
(JR: I’m not going to write this up from my notes at this point, but instead just leave the headings as placeholders.)
a) Patient privacy and confidentiality.
b) Securing your own Internet presence.
c) Boundaries of the patient-physician relationship.
d) Separating personal and professional content online.
e) Colleagues violating professional norms on social media.
f) Reputational harm to the profession, not just you.
g) Does your social media presence amount to “canvassing or touting”, especially when you criticise other medical professionals?
h) Don’t just spread information that you already agree with. Be careful and skeptical. Don’t treat anecdotes as if they are data.
Noakes and the HPCSA
(Contains much copy/paste from previous columns.)
In his column entitled “The Digital Doctor” from Big Issue: Noakes tells us that “now it is only the advice that works that has long-term credibility”, and that is true, up to a point. The problem is that harms can occur in the short-term, while “long-term credibility” is being established.
And, it is of course true that you will usually get caught out on social media if you spread misinformation. But that doesn’t mean information gains credibility through being widely disseminated (on channels you’ve hand-picked) on social media. Those are separate issues.
It’s also true that professionals – in various spheres – were able to exploit the ignorance of the consumer to peddle quackery or defective goods, and that they are now less able to do so than in the past. But our easier access to information doesn’t mean that (proper) experts don’t often know better than we do. Those are also separate issues.

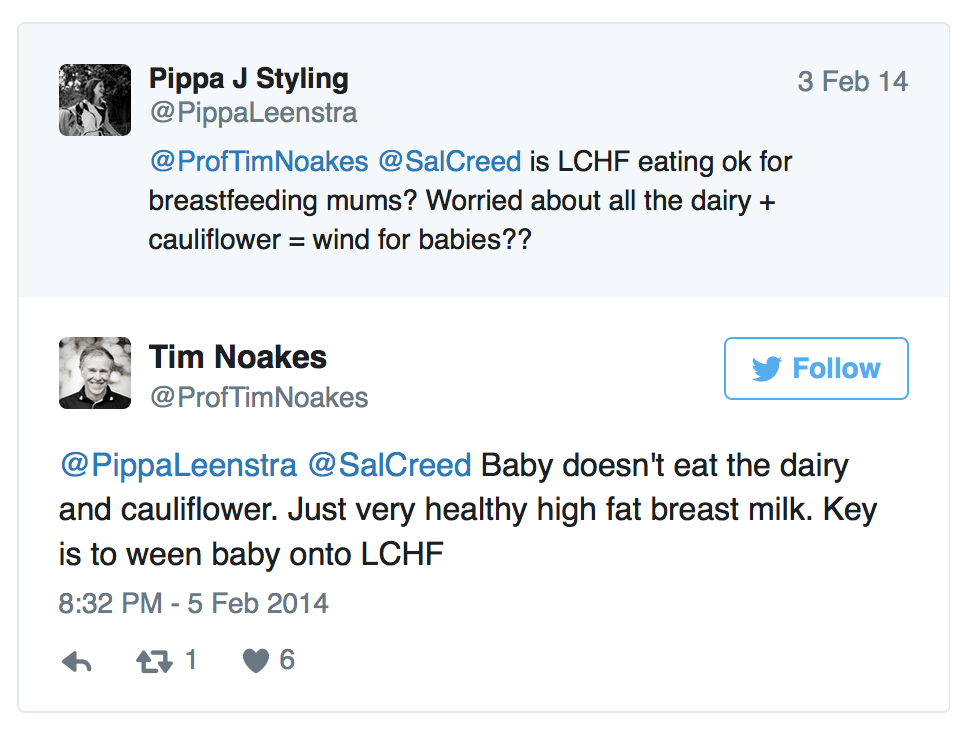
But in the case of this particular tweet, I’m not convinced of any ethical breach (a separate issue to a violation of common sense, of course), seeing as I don’t believe that she was a patient. The breach of common sense, though, is in the fact that Prof. Noakes should be well aware of his role and perceived authority, as per the two principles discussed earlier.
The same tweet, but with some sort of disclaimer that (in Goldacre’s words) “it’s a little more complicated than that” would be the least you’d expect.
As a simple example of how it’s a little more complicated (at least) imagine the confusion of a “patient” reading the above, but who has also read this (since deleted) from the “Real Meal Revolution Website”:

So, I’d call this irresponsible, but not unethical, at least not as per the current rules. But it’s easy to find tweets from Prof. Noakes that are to my mind unethical, such as ones that endorse vaccine/autism pseudoscience, or direct people to known quack websites.
Should this hearing be happening at all?
(What followed was an oral version of chunks of this post, which I won’t reproduce here.)
In closing, remember that your intentions are only part of the story – people hear what they want to. So consider the worst outcome imaginable – the worst misreading, the most unfortunate consequences (including what might happen if you’re wrong), not the best!
(Followed by a few examples of my being misread on social media, and the humorous/scary/bizarre responses that has lead to.)